Office Workers Have 38% Higher MSK Rates Than Laborers And Other Workforce Health Assumptions Your Data Is Busting

Think back pain is a blue-collar problem? Think again.
New data from Nomi Health reveals a counterintuitive trend: white-collar employees, ie. those in office-based, professional roles, report significantly higher rates of musculoskeletal (MSK) disorders than their blue-collar counterparts.
In a national analysis of 435 employers, employees behind desks showed 38% higher MSK rates than skilled laborers. Across the board, 27% of office workers report incidents of back pain, compared to just 18% in physical jobs.
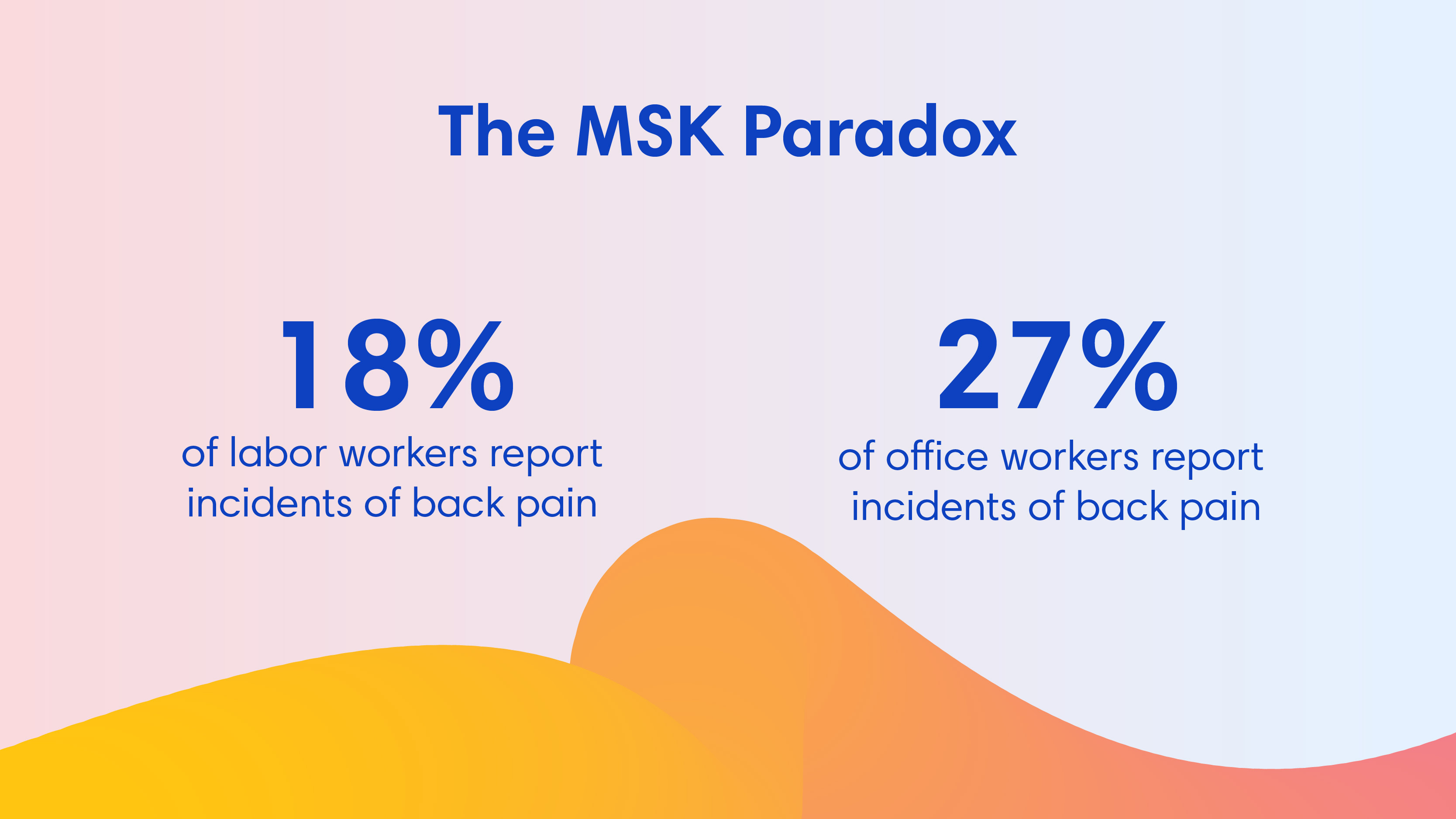
This is the MSK Paradox. And it challenges decades of assumptions about workplace health.
Why Job Title Is a Poor Predictor of MSK Risk and Healthcare Costs
Companies have long treated job titles as proxies for health risks. Construction workers get injured. Office workers get stressed. Retail workers have high turnover. But today’s workforce doesn’t fit those neat categories. And neither does their healthcare use.
To better inform healthcare strategy, Nomi Health developed a data science model that moves past industry codes, job titles, and employer stereotypes, to focus on healthcare behavior and consumption. The model analyzed healthcare engagement across more than 400 companies and found that workforce behavior grouped companies into nine distinct archetypes.
The result: a 95.4% match rate between each company’s behavior and its assigned archetype.
The Nine Workforce Healthcare Archetypes And Why Industry Codes Miss the Point
These archetypes go beyond where people work to reveal how they use care, as we see. the MSK paradox.
Nomi's model surfaces another surprising trend: high salaries don’t always signal better social determinants of health (SDoH).
Why Finance Workers Score Worse on Economic Security Than Retail Workers — Despite Earning 3× More
It’s easy to assume that high salaries lead to financial stability and social well-being. But the data tells a different story.
Finance workers earn nearly three times more than retail employees: $131,665 vs. $46,448. Yet they also score worse on economic insecurity risk and overall SDoH scores (Social Determinants of Health Risk).
- Economic insecurity score: 41.8 (finance) vs. 38.8 (retail)
- Overall SDoH risk score: 40.4 (finance) vs. 38.6 (retail)
(Higher numbers indicate greater barriers.)
At the same time, finance workers have better access to healthcare and digital services, highlighting the layered, and sometimes contradictory, reality of social risk.
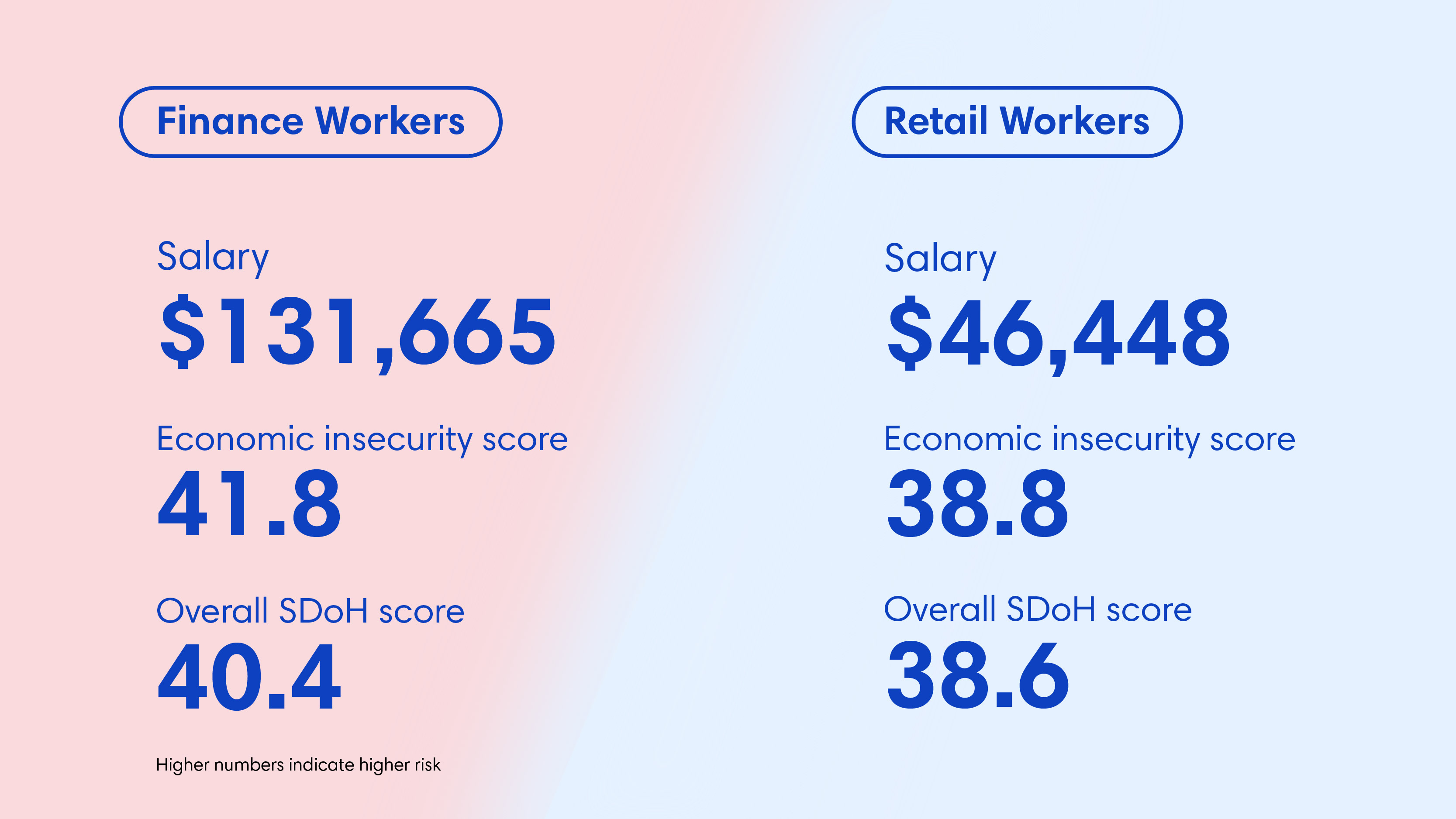
This finding turns a core assumption on its head: that income predicts security. In reality, job type and work environment create social patterns that salary can’t explain.
Behavior tells the real story. Income is just a subplot.
Why Industry Benchmarking Leads Employers to Overspend on the Wrong Health Programs
Most employers still compare themselves to others in their industry. Manufacturers benchmark against other manufacturers. Tech against tech. But that broad-brush approach hides what’s really happening inside the workforce.
Two employers might share an industry code and headcount but have completely different care patterns. One might be full of “Proactive Care Consumers” who demand flexibility and digital tools. The other might be “Healthcare Pragmatists” who care more about efficiency and cost.
When your strategy ignores those differences, your outcomes suffer. You overspend on the wrong programs. You underinvest in the right interventions. And you miss the chance to improve workforce health.
How Behavior-Driven Benefits Strategy Outperforms Traditional Industry Benchmarks
Nomi’s archetype model delivers three immediate advantages for forward-looking employers:
1. Speed to strategy: Identify your healthcare archetype in minutes, not months. Get early visibility into cost drivers and utilization patterns, without waiting for year-end claims.
2. Precision targeting: Benchmark your performance against companies that behave like yours, not just those that share your label.
3. Predictive planning: Design your next moves based on the proven behavioral patterns of similar employers, even while deeper analysis is still underway.
Employers using archetype-driven strategy are already optimizing for what’s next, while others are still reviewing last year’s data. Understanding healthcare behavior helps you move faster, plan smarter, and connect benefits to behavior.
The takeaway?
Don’t just update your benefits. Upgrade your lens.
What's the Right Healthcare Archetype for Your Workforce?
The MSK paradox is just the beginning.
Uncover the full story behind your healthcare data at g.nomihealth.com
Frequently Asked Questions
Do office workers really have higher MSK rates than laborers?
Yes, and by a significant margin. Nomi Health analysis of 435 employers found that office-based employees report MSK disorders at rates 38% higher than skilled laborers. 27% of office workers report back pain incidents compared to 18% in physical jobs. Prolonged sitting, sedentary posture, and repetitive low-level strain appear to create more cumulative MSK burden than many physically demanding roles.
Why do white-collar employees have higher musculoskeletal disorder rates?
The data doesn't pinpoint a single cause, but the pattern is consistent across more than 400 companies. Office environments involve prolonged sitting, static postures, and repetitive low-intensity strain that accumulate over time differently than the more variable physical demands of labor roles. Traditional workplace health assumptions — that physical jobs carry higher injury risk — don't hold up in actual claims data.
What are workforce healthcare archetypes and how do they help employers?
Workforce healthcare archetypes group employees by how they actually use healthcare, drawing on real claims patterns across more than 400 companies. Nomi Health's model analyzed healthcare engagement across more than 400 companies and identified nine distinct archetypes with a 95.4% match rate. Archetypes help employers benchmark against companies that behave like theirs, identify cost drivers earlier, and design benefits programs that match how their workforce actually seeks care.
Why don't industry benchmarks always accurately predict healthcare costs?
Two employers can share an industry code and headcount but have completely different care utilization patterns. Benchmarking against others in your industry assumes shared behavior that often doesn't exist. One manufacturer might employ proactive care seekers who want digital tools and flexibility. Another might employ cost-focused pragmatists. A strategy built on industry averages may overspend on the wrong programs and miss the interventions that would move the needle.
Do higher salaries predict better workforce health outcomes?
Not reliably. Nomi Health data shows finance workers earning nearly three times more than retail employees ($131,665 vs. $46,448) but scoring worse on economic insecurity and overall social determinants of health risk. Finance workers score 41.8 on economic insecurity versus 38.8 for retail workers. Income is one factor, but job type, work environment, and social patterns create health dynamics that salary alone doesn't predict.
How can employers identify their workforce healthcare archetype?
Nomi Health's archetype model can identify a company's healthcare archetype quickly and provide early visibility into cost drivers and utilization patterns without waiting for year-end claims data. Employers can start at g.nomihealth.com to learn more about their workforce's behavioral profile.



